In the practice of facial aesthetic medicine and surgery, isolated treatment of a single region is rarely aesthetically pleasing without ultimately considering other facial regions for harmonization. While this treatment philosophy seems obvious, somehow tear trough deformity (TTD) correction has been traditionally addressed in isolation. In this article a more global and inclusive treatment approach is proposed for the correction of TTD.
Although it may be part of a natural appearance in youth, many patients express concern about the impression of a somewhat gaunt appearance consequent to tear trough hollowing. TTD may it may appear in isolation but usually manifests as a component of general mid-face insufficiency. As opposed to malar fat in the cheek region, lower lid subcutaneous fat is virtually non-existent, permitting seamless lid mobility in its ocular function. Furthermore, a subtle demarcation between the lid and the cheek is natural. However, with age related regional bone regression, a tear trough in the medial aspect of the lid-cheek junction may be perceived as a “deformity”.
Attempts at surgical and non-surgical correction of a TTD can prove deceptively challenging. A TTD is underrated in its complexity. Furthermore, in cases of superficial hyaluronic filler placement, the objective of an aesthetic improvement in the region can be complicated by persistent nodularity, oedema and Tyndall effect that in turn can often prove treatment resistant. Bruising and skin discolouration can further complicate matters. These complications can prove unsightly and distressing to the patient and can even interfere with normal lower eyelid function.
The most serious potential complication when injecting fillers in the periorbital region is the risk of intra-vascular injection with consequent tissue damage (Nicolau syndrome or embolia cutis medicamentosa) and rarely blindness. The infra-orbital and angular arteries and their branches in the tear trough region are more vulnerable than commonly appreciated.
Accordingly, in TTD corrective procedures, patient dissatisfaction is quite common and often in concert with that disaffection is treating physician despair! In the end it can be both the patient and the physician who share “blood sweat and tears” rather than the mutual satisfaction of a pleasing treatment TTD outcome.
Hirmand (1) classified patterns of periorbital volume loss that acknowledged the TTD as only part of the mid-face insufficiency:
Class I: limited to the tear trough or medial orbit (sometimes associated with very mild flattening of the central cheek).
Class II: medial and lateral depression apparent (can be associated with mild volume deficiency in the medial cheek and mild flattening of the central triangle.
Class III: full depression visible circumferentially at the orbital rim (often associated with more advanced volume deficiency in the medial cheek, central reverse triangle/midface and malar eminence, and the oblique mid cheek crease highlighting the malar bags).
Treatment of Tear Trough Deformity
Historically, Lambros (2); Kane (3); Stutman/Codner (4); K & S Steinsapir (5); Patel/Glaser (6); Hussain SN et al (7) and many others have described various techniques using injectable fillers for TTD correction. However, Galadari & Redka-Swoboda were probably the first practitioners to recognise and reference TTD treatment as only part of the total regional insufficiency. They recently described an advanced and relatively atraumatic single-entry point cannula method to deliver injectable filler from a lateral cheek perspective, addressing the malar cheek and tear trough deficit in its entirety.(8)
Similar to the experience of Galadari/Redka-Swoboda and extrapolating from a long experience with fat transfer grafting to the deep cheek fat pads, the author observed that volumizing the deep cheek fat compartment with rheologically matched hyaluronic fillers, not only improved the malar region but also improved other regional aesthetic targets including the lid-cheek junction.(9)
Method
The author utilises an entry point at the intersection of two imaginary lines, one line drawn from the upper tragus to the alar groove and a second being a perpendicular line extending downwards from the lateral orbital rim.
After injecting a small bleb of Lignocaine 1% with a 30g needle at the entry point, a 21g needle is introduced to create an adequate entry access for the subsequent insertion of a 23g, single hole 50mm cannula. The cannula is attached to a 5ml syringe loaded with ~0.3% Lignocaine solution. The deep malar fat pad compartments (and also tissue supero-lateral along the upper aspect of the Zygomatic process) are gently hydro-dissected with the local anaesthetic solution. Subsequently, using the same 23 g cannula, a rheologically appropriate quantity (e.g.~1 ml) of a volumizing hyaluronic filler is injected in multiple passes to fill the sub-SMAS mid cheek fat pads (SOOF, Medical & Lateral Deep). A small quantity (e.g.~0.2ml) is injected supero-laterally immediately superior to the Zygomatic process and via the temporal tunnel into the lower temporal compartment.
Soon after the injection of the filler, the region is gently massaged, including “milking” some of the injected filler superiorly towards the orbicularis retaining ligament and tear trough ligament. Thereby the entire deep malar complex, plus the lower temporal compartment and any associated TTD is addressed. Using this method, it is actually quite uncommon to require any subsequent, specific subcutaneous filler placement at the TTD. The advantages of this approach are many, including minimising risk of complications such as bruising, subcutaneous nodules, subcutaneous oedema, lower lid oedema, Tyndall effect and vascular occlusion.
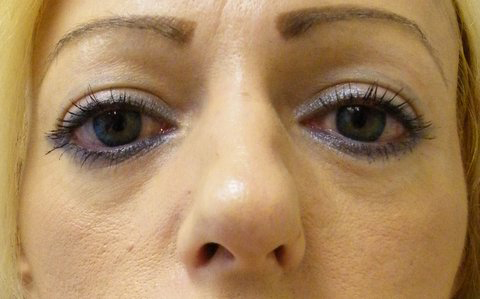
Figure 1: The "before" photo
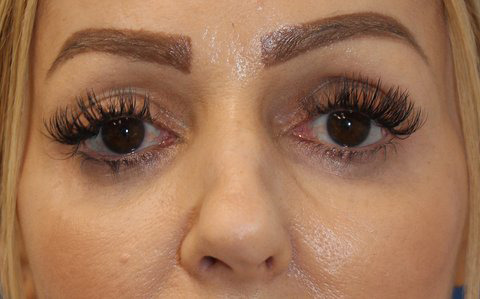
Figure 2: The "after" photo
Moreover, the regional retaining ligaments are supported and re-tensioned with correction of the TTD, shortening of the lower lid lash-orbital rim distance and regression of any concurrent lower lid fat herniation. There is also a concurrent supero-lateral vector lifting effect of the malar region and lateral canthus consequent to the supero-laterally placed filler. Aesthetically pleasing ogee midface cascading curves are enhanced at the lid-cheek junction, cheek and the malar-buccal junction. Midface phi-ratio proportions are often improved along with the ideal (in females) of a heart shaped formation from the midface down into the lower face.
Summary
The author suggests consideration of a regional rather than an isolated approach to injectable filler correction of a TTD.
References:
(1) Hirmand, H; Anatomy and nonsurgical correction of the tear trough deformity. Plast Reconstr Surg 2010;125(2):699-708.
(2) Lambros VS. Hyaluronic acid injections for correction of the tear trough deformity. Plast Reconstr Surg. 2007;120:74S–80S
(3) Kane MA. Treatment of tear trough deformity and lower lid bowing with injectable hyaluronic acid. Aesthetic Plast Surg. 2005;29:363–7.
(4) Stutman RL, Codner MA. Tear trough deformity: Review of anatomy and treatment options. Aesthet Surg J. 2012;32:426–40
(5) Steinsapir KD, Steinsapir SM. Deep-fill hyaluronic acid for the temporary treatment of the naso-jugal groove: Ophthal Plast Reconstr Surg. 2006;22:344–8
(6) Glaser DA, Patel U. Enhancing the eyes: Use of minimally invasive techniques for periorbital rejuvenation. J Drugs Dermatol. 2010;9:S118–283
(7) Hussain SN, Mangal S, Goodman GJ. The Tick technique: A method to simplify and quantify treatment of the tear trough region. J Cosmet Dermatol. 2019;18:1642–1647
(8) Galadari, Redka-Swoboda. Injection of filler for volume replacement of the whole face using a single-entry method. Journal of the American Academy Dermatology, Volume 77, Issue 6, e163 - e164
(9) Feiner R, C Bouzouaya C; Suture Lifting and Liposculpture Integration in the Creation of Facial Esthetic Harmony, Miniinvasive Face and Body Lifts - Closed Suture Lifts or Barbed Thread Lifts, Nikolay Serdev, Intech Open, DOI: 10.5772/51246
Marcado: Injeções
Compartilhe esse artigo em


