Abdominal adiposity reduction with Drakarian: results from three clinical cohorts (deviceonly, +exercise, +Mediterranean diet)
Introduction
Abdominal adiposity is clinically relevant because visceral adipose tissue (VAT) exhibits a stronger association with adverse metabolic risk factors than subcutaneous adipose tissue (SAT), despite both compartments correlating with cardiometabolic risk. ¹ This distinction matters in practice because weight and BMI can miss meaningful differences in fat distribution and associated risk.
For outcome reporting, imaging-based quantification provides compartment-specific endpoints. In methodological literature, CT and MRI are treated as reference standards for quantifying intra-abdominal adipose tissue, with MRI offering the advantage of not requiring ionizing radiation. ² MRI-based segmentation approaches are widely used for the measurement of VAT and SAT volumes in research settings. ³
This article synthesizes findings from three Drakarian-based cohorts:
- (i) a published device-only study assessing anthropometrics and MRI-derived SAT outcomes, ?
- (ii) a published device + exercise study assessing MRI-derived VAT/SAT and metabolic markers, ?
- (iii) an unpublished internal cohort (Mediterranean diet + Drakarian; 12 sessions, 1 hour, 2×/week; n=20) analysed as baseline?final change. Each cohort will be presented in a visual-first module (photo + compact table + key figure), followed by a cross-cohort comparison.
Study 1 — Drakarian only (published)
Study snapshot
This prospective pre–post cohort evaluated a high-power second-generation TECAR protocol. The device operated at 1 MHz (maximum 1240 W) with four channels, regulating delivered energy by measuring patient absorption. Treatment consisted of 80 minutes at 50°C, delivered as 10 sessions over 2 weeks (continuous sessions except Saturday/Sunday). Outcomes included waist measurement and MRI-based analysis of abdominal subcutaneous fat, with lipid profile assessed at baseline and end of treatment.4A representative before/after is presented in Figure 1, while key outcomes are summarized in Table 1 and the change in MRI-derived subcutaneous fat mass (g) is illustrated in Figure 2.
Table 1. Study 1 key outcomes (baseline ? final)
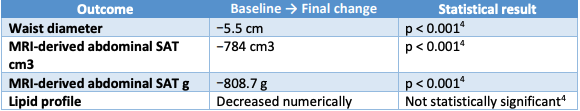
Outcome Baseline ? Final change
Figure 1. Representative baseline vs end-of-protocol clinical image before (A) and after (B) from the device-only cohort.
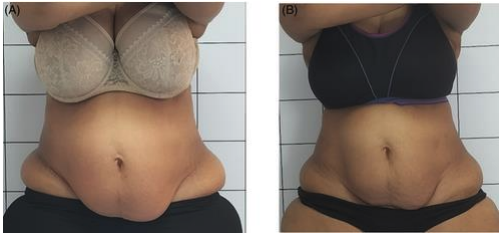
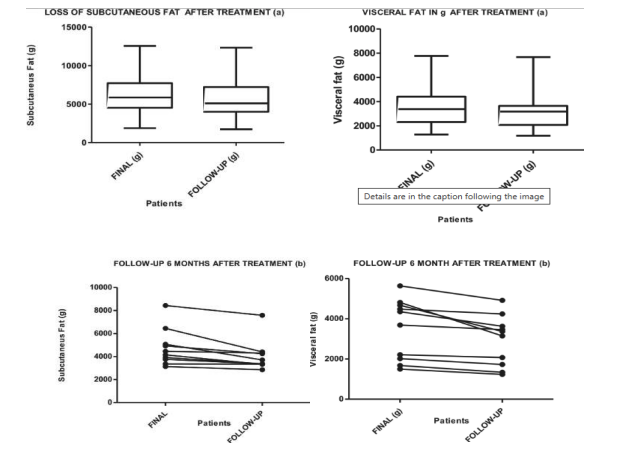
Figure 2. MRI-derived abdominal subcutaneous fat (SAT) mass (g) at baseline and final
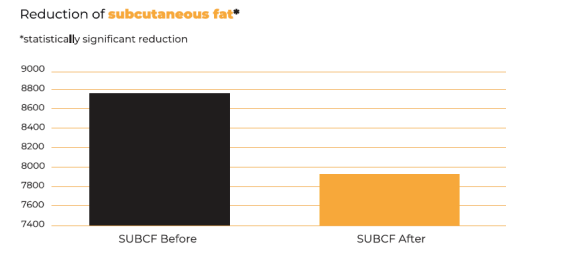
Interpretation
In the device-only cohort, the Drakarian protocol was associated with a statistically significant reduction in waist measurement and MRI-derived abdominal subcutaneous fat at the end of treatment, while lipid markers showed non-significant downward trends.
Study 2: Drakarian + exercise (published)
Study snapshot
This pilot pre–post study included 34 participants (17 women, 17 men) who completed a 10-day intervention (weekday sessions; no sessions on Saturday/Sunday). Each session used an abdominal belt covering 800 cm² to deliver amplified radiofrequency energy, followed immediately by 45 minutes of submaximal aerobic exercise. Outcomes were assessed pre- and post-intervention, including MRI-quantified abdominal fat (VAT and SAT in cm³ and grams), anthropometrics, lipid profile, metabolic markers (glucose, insulin, leptin), and CRP. The low levels of C-reactive protein confirm that there are no inflammatory effects. A follow-up assessment was performed at 6 months. ? A representative before/after is presented in Figure 3, while key outcomes are summarized in Table 2 and MRI-derived adiposity changes are illustrated in Figure 4.?
Table 2. Study 2 key outcomes (baseline ? final) ?
(Values are mean; p-values from pre–post comparisons reported in the article.)
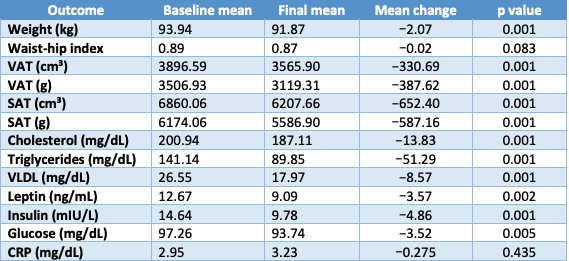
Figure 3. Representative clinical images (female) at baseline (b), post-intervention at day 10 (a), and 6-month follow-up (6 m) in the Drakarian + exercise cohort. ?
Figure 4. MRI-derived SAT and VAT mass (g): end of treatment vs 6-month follow-up. ?
Interpretation
The combined protocol produced statistically significant reductions in MRI-derived VAT and SAT (both cm³ and grams) and improvements in several metabolic/lipid markers (e.g., triglycerides, VLDL, insulin, leptin), with no serious adverse events reported beyond transient skin redness. ? At 6-month follow-up, the paper reports maintenance of fat loss without restoration of VAT or SAT.?
Study 3: Drakarian + Mediterranean diet (unpublished internal cohort)
Study snapshot
This internal cohort assessed a combined protocol of Mediterranean diet + Drakarian delivered as 12 sessions (1 hour/session, 2 sessions/week). Outcomes were analysed as baseline ? end of treatment changes for anthropometrics (weight, BMI), MRI-derived abdominal adiposity (VAT and SAT in cm³ and g), and selected blood markers. ? A representative before/after is presented in Figure 5, while key outcomes are summarized in Table 3 and MRI-derived adiposity changes are illustrated in Figure 6.?
Table 3. Study 3 key outcomes (baseline ? final), n=20 ?
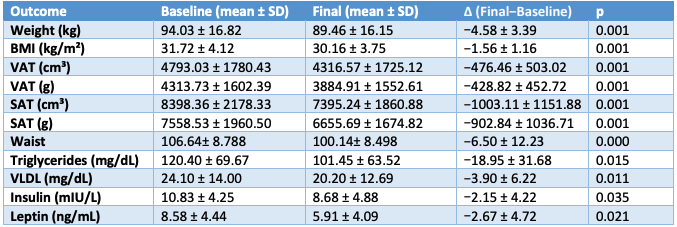
Figure 5. Representative clinical images at baseline, end of treatment, and 3-month follow-up in the Mediterranean diet + Drakarian cohort.
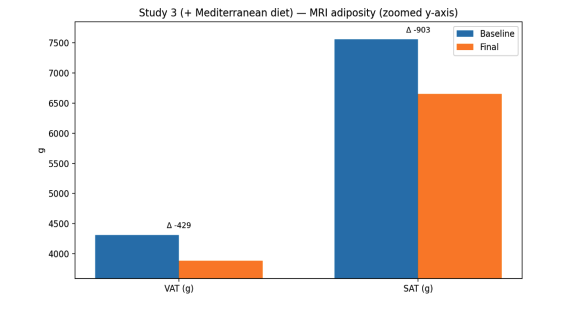
Figure 6. MRI-derived visceral and subcutaneous fat mass (VAT and SAT, g) at baseline and final in the Mediterranean diet + Drakarian cohort.
Conclusion
Across three cohorts, Drakarian-based protocols were associated with consistent reductions in abdominal adiposity. The device-only cohort demonstrated significant reductions in waist measurement and MRI-derived subcutaneous fat. The exerciseadjunct cohort showed statistically significant reductions in both visceral and subcutaneous fat, alongside improvements in several metabolic markers, with followup figures suggesting maintenance at 6 months. In the Mediterranean diet–adjunct internal cohort (n=20), significant reductions were observed in weight, BMI, visceral fat, and subcutaneous fat, with additional improvements in triglycerides/VLDL and insulin–leptin profiles.
Overall, these findings support a practical interpretation: device-only protocols provide measurable changes in anthropometrics and subcutaneous fat, while adding structured lifestyle measures (exercise or Mediterranean diet) may enhance clinically relevant outcomes, particularly visceral fat and metabolic markers. Future work should prioritize larger comparative designs, standardized MRI endpoints, and predefined follow-up intervals to confirm durability and identify responder profiles.
REFERENCES
- 1. Fox CS, Massaro JM, Hoffmann U, Pou KM, Maurovich-Horvat P, Liu C-Y, et al. Abdominal visceral and subcutaneous adipose tissue compartments: association with metabolic risk factors in the Framingham Heart Study. Circulation. 2007;116(1):39-48. doi:10.1161/CIRCULATIONAHA.106.675355.
- 2. Murphy J, Bacon SL, Morais JA, Tsoukas MA, Santosa S. Intra-Abdominal Adipose Tissue Quantification by Alternative Versus Reference Methods: A Systematic Review and Meta-Analysis. Obesity (Silver Spring). 2019. doi:10.1002/oby.22494.
- 3. Hu HH, Nayak KS, Goran MI. Segmentation and quantification of adipose tissue by magnetic resonance imaging. Magnetic Resonance Materials in Physics, Biology and Medicine. 2011/2015 (review available in PMC).
- 4. Rodríguez Lastra J, García Cardona Y. Loss of subcutaneous fat in 20 patients, both sexes, using a second-generation TECAR device of 1,240 Watts and results analyzed with magnetic resonance. J Cosmet Dermatol. 2024;23(3):869-875. doi:10.1111/jocd.16078.
- 5. Rodriguez Lastra J, Kouser S. Reduction of Subcutaneous and Visceral Fat With the Use of Energy-Based Equipment With a High-Power Amplifying Effect Plus an Exercise Regimen. J Cosmet Dermatol. 2025;24(10):e70490. doi:10.1111/jocd.70490
- 6. Rodríguez Lastra J, Kouser S. Drakarian + Mediterranean diet cohort (diet arm; n=20): baseline to end-of-treatment outcomes. Unpublished data
Author Disclosure: Sidra Kouser works as clinical researcher for Capenergy Medical, manufacturer of the Drakarian device, subject of this article.
Learn more at www.capenergy.com
Tagged: Lasers, EBD & body shaping
Share this article on


