Management of Perianal Intertrigo with Secondary Infection: A Case Study on the Effectiveness of Combined Topical Therapy
Introduction
Intertrigo is a superficial inflammatory skin condition that commonly appears in flexural areas such as the axillae, inguinal folds, inframammary region, and perianal area. Factors such as moisture, friction, and poor ventilation contribute to its development(1,2). Secondary infections, primarily by Candida spp. and occasionally Staphylococcus aureus, may complicate the condition(3). Diagnosis is primarily clinical, but complicated cases may require additional testing such as microscopy, culture, and dermoscopy. Prompt recognition and appropriate management are essential to prevent complications.
Pathophysiology and Epidemiology
Intertrigo results from continuous skin-to-skin friction, especially in the presence of moisture. The warm and humid environment in skin folds facilitates epidermal maceration and microbial proliferation. Risk factors include obesity, diabetes mellitus, and poor hygiene(1). Intertrigo is more common in warm and humid climates and can affect individuals of any age, gender, or ethnicity (2).
Case Report
A 25-year-old female presented with erythema, pruritus, discomfort, and local irritation in the perianal region, which developed during the last two days of a 9-day course of Amoxiclav. The patient had also been using menstrual pads due to her menstrual cycle.
The clinical diagnosis was intertrigo with secondary fungal infection, based on visual examination and reported symptoms.
Treatment protocol:
- Local cleansing with chamomile tea.
- Drying with gentle compresses.
- Topical cream application containing:
-Triamcinolone acetonide (anti-inflammatory corticosteroid),
-Neomycin (broad-spectrum antibiotic),
-Nystatin (antifungal active against Candida spp.).
Dosing: Twice daily in the first week, once daily in the second week.
Results
After 7 days, a noticeable reduction in erythema and pruritus was observed. After 14 days, the patient reported complete symptom resolution with no adverse effects.
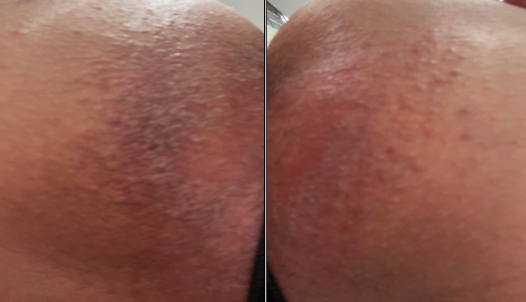
Fig.1: Initial presentation of perianal intertrigo with erythema, maceration, and signs of secondary fungal infection.
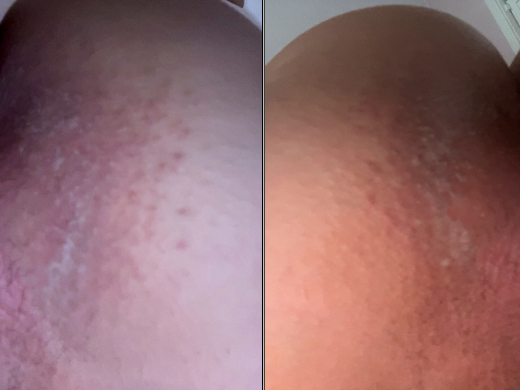
Fig.2: Day1 of treatment with combined topical cream containing triamcinolone, neomycin, and nystatin: inflammation and discomfort still evident.
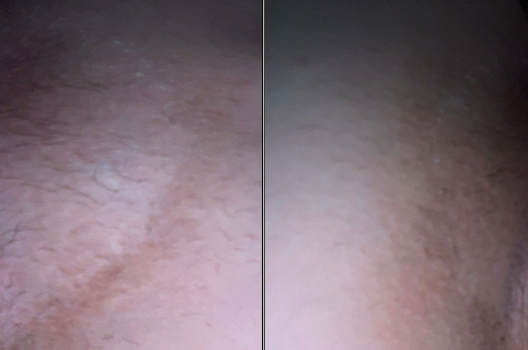
Fig.3: Day 7 of treatment: noticeable improvement in erythema and reduction in pruritus.
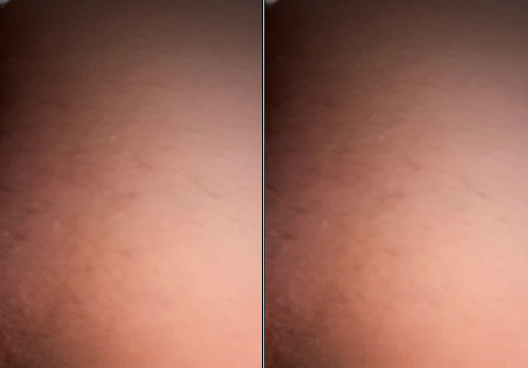
Fig.4: Day 14 of treatment: complete resolution of clinical signs with restoration of skin integrity.
Discussion
The management of complicated intertrigo presents clinical challenges, particularly when associated with microbial infections. Combined topical therapy with anti-inflammatory, antibacterial, and antifungal components can address the full pathogenesis of the condition and facilitate rapid healing. Triamcinolone reduces inflammation, while neomycin and nystatin target bacterial and fungal infections, respectively.
This case underscores the value of an integrated approach in managing intertrigo and supports the use of combination creams as a first-line treatment, in conjunction with hygiene measures and avoidance of irritants(3).
Conclusion
This case report demonstrates the efficacy of combined topical treatment with triamcinolone, neomycin, and nystatin in managing perianal intertrigo with secondary infection. Complete clinical improvement within two weeks and absence of side effects suggest that this regimen is a safe and effective option. Emphasis should also be placed on individualized therapy tailored to the underlying etiology.
References
1. Janniger CK, Schwartz RA. Intertrigo and common secondary skin infections. Am Fam Physician. 2005.
2. Leman JA, Holden CA. Intertrigo. Clin Exp Dermatol. 2002.
3. Gupta AK, Bluhm R. Topical antifungal agents for the treatment of tinea infections. Drugs. 2004.
Etiquetas: Dermatología clínica & cirugía dermatológica
Share this article on


