Non-surgical Rhinoplasties: Is Cannula Safer Than Needle in Ethnic Patients?
Non-surgical rhinoplasties may seem like a quick and simple solution with hardly any downtime. There are two well-known non-surgical treatments for nose reshaping either with hyaluronic acid filler or with absorbable threads like PDO and in combination of both. But tailoring the treatment plan to each individual's unique nasal structure is crucial. As an injector who works with both Caucasian and Asian/ethnic patients for non-surgical rhinoplasties, I've learned that to achieve the best outcomes require a deep understanding of every technique and the anatomy of the nose. While HA filler is a common treatment option, it's not always the best choice for every patient.
At IMCAS World Congress 2024 Main Stage, non-surgical rhinoplasty was a hot topic this year. Esteemed panels shared their individual thoughts on technique and safety, including the use of cannula versus needle for delivering treatment. While published papers have cited the safety of cannula technique, Dr. Hong Ha Nguyen presented a talk on blindness after rhinoplasty that left the room in silence. Surprisingly, almost all the blindness cases resulting from non-surgical rhinoplasties were caused by cannula technique.
As a practitioner who has been treating both Caucasian and ethnic nasal structures, I can see why this is happening. It's important to question the nasal structures of the models recruited in the studies. The rate of complications reduces with cannula technique in Caucasian noses with high bridges, humps, bumps, deviation, and hook appearances. Unfortunately, this is not what we see when it comes to Asian/ethnic noses whereby cannula was used in all the cases of blindness presented by Dr. Nguyen.
So, should we stop using cannula altogether? Or should we stop treating the nose entirely?
As medical professionals, we know that a thorough assessment is crucial before diagnosing and treating any condition. This includes inspecting, palpating, and auscultating (use of ultrasound will be in this case), as well as taking a detailed history. When it comes to treating nasal deformities, history taking is important and should include addressing any congenital or acquired deformities, previous trauma or surgeries, previous non-surgical treatments, underlying autoimmune disorders, medications, and history of allergies.
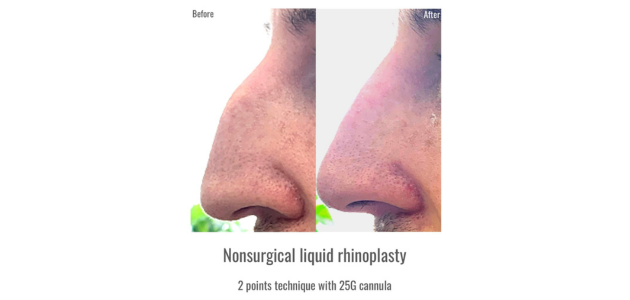
By carefully inspecting and palpating the nasal structures and surroundings, providers can determine the most appropriate technique and use the best tools for each particular case. It's important to note that there is a difference between the "best" tools and the tools you know best. Using a gel substance (HA) to heighten and create a nice bridge border may not always yield the safest or best outcomes. Most providers opt for cannula, especially in flat noses, to minimise risks. However, a high G prime HA may necessitate a significant amount, leading to a wider nose, which is not ideal. In the worst-case scenario, attempting to create a border in a confined space could pose risks of vascular compression or even lead to accidental vessel cannulation and catastrophic outcomes like blindness as shared by Dr. Nguyen.
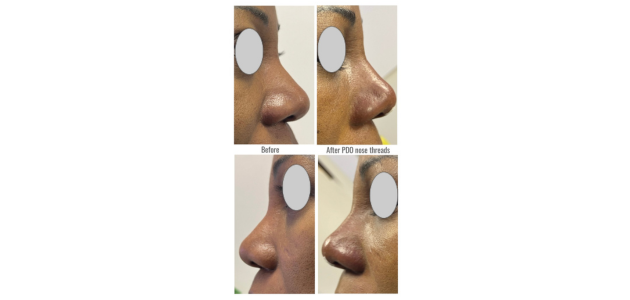
In my practice, utilising PDO threads in ethnic nose cases, sometimes in conjunction with HA filler, has consistently produced excellent results without complications. Ethnic noses present challenges due to tight spaces between bones and skin, as well as varying skin thickness. The use of solid materials like threads helps create a more stable foundation, effectively lifting the skin and enhancing the nasal septum compared to HA fillers.
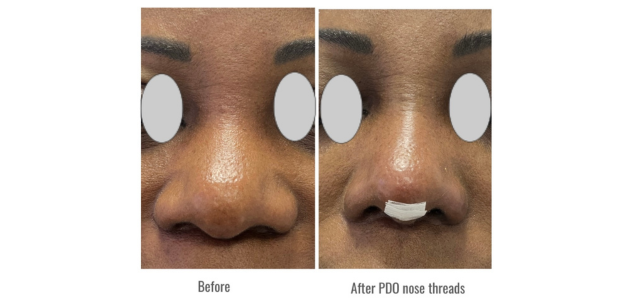
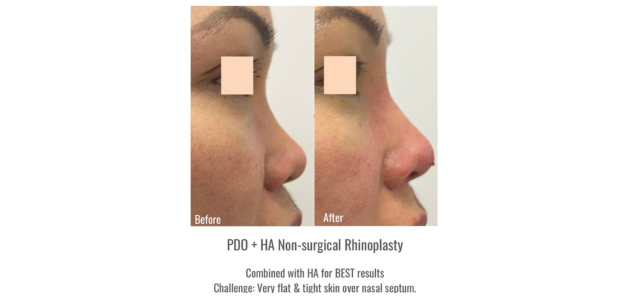
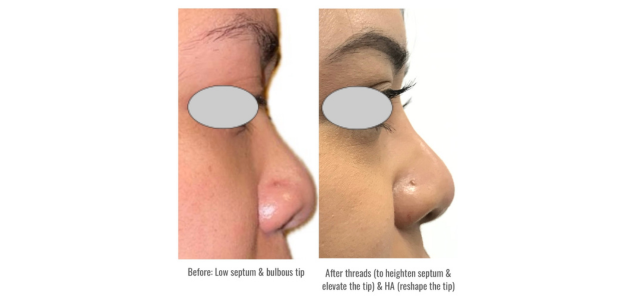
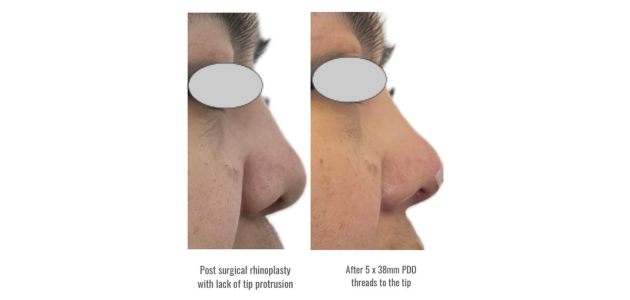
For instance, in a case of post-rhinoplasty with cartilage but tip insufficiency, inserting five 38mm PDO threads from the tip to the base/anterior nasal spine resulted in significant tip protrusion. The threads approach not only improves flat bridges but also elevates bulbous tips, leading to a slimmer and more aesthetically pleasing appearance that lasts longer than HA fillers.
Last but not least to me, practically and technically having a universal tool is the ultimate key to safer, satisfactory and much more favourable outcomes. This will include the usage of HA filler, threads or combinations of both. I look forward to sharing my insights on this topic at the upcoming meeting to collectively explore the best approaches with my colleagues and strive towards safeties for all.
Mots-clés: Injectables, Fils tenseurs
Partagez cet article sur


