The growing importance of ultrasonography in cosmetic dermatology: An update after the 23rd IMCAS Annual World Congress (2022)
Abstract
Background
Ultrasound (US) has been used for many years in the field of medicine. Many specialties have embraced US as a quick, painless, and relatively inexpensive tool to assist the clinician in determining anatomy, pathology, and aid in diagnostic or therapeutic procedures. US allows for precise mapping of cutaneous and subcutaneous structures in the face, in particular vascular structures. The use of US leads to reduced chances of complications and clinical failures, rendering more safety and high quality.
Methods
US is considered the first-imaging technique for dealing with fillers and managing their potential complications. US can be deployed for vascular mapping, safe placement of fillers, and directed low-dose hyaluronidase reversal of vascular adverse events. It is a noninvasive imaging modality that provides a good definition for studying the skin, deeper layers, and blood flow in real time. In other words, we go from static to dynamic anatomy. In addition, US can guide with the application of botulinum toxin, in order to define the muscular planes. US may contribute to a more personalized procedure, better cosmetic results, and help to avoid complications. In general, physicians tend to use it for prevention. Last, for research purposes, US examination provides valuable information on the behavior, longevity, and interaction of the filler within the tissues.
Conclusion
This new approach for US-guided treatments is a very practical and an effective method in cosmetic dermatology. As doctors, we owe it to our patients to do our best to prevent any harm. We feel that in near future, US will be an essential diagnostic tool in any dermatology or cosmetic doctor's office to both ensure safety and provide legal protection for the professional.
INTRODUCTION
The field of medicine has benefited vastly from ultrasound (US) technology. Many medical specialties have embraced US because it is a quick, painless, and relatively inexpensive tool to assist the clinician in determining anatomy, pathology, and aid in diagnostic or therapeutic procedures. US was first introduced in clinical dermatology in 1979. 1 The field of cosmetic dermatology, however, started much later on using US as an important tool. 2,3 US allows for precise mapping of cutaneous and subcutaneous structures in the face, in particular vascular structures. 2 In turn, this knowledge enables the professional to carry out their task in a safe manner. Plus, the use of US leads to reduced chances of complications and clinical failures, rendering more safety and high quality. 4
US has not been routinely used in cosmetic dermatology due to several reasons, such as large equipment, low-definition images, costs, and availability. 5 The miniaturization reduced costs and especially higher megahertz frequencies providing improved quality of superficial tissue layer imaging have eradicated the previously mentioned problems. 6 Simply put, modern era US devices are small, portable, practical, with high frequency and increasingly affordable. Portable wireless probes connectable to smartphones or tablets including software are offered at a fair price and are now easily available. 7
1.1 Ultrasound in cosmetic dermatology: how?
The US transducer (also named probe) emits a sound wave which is reflected by the examined tissue while the echo is detected by the transducer. Practically, the transducer is both transmitter and receiver of US. There are various probes including linear, convex, and phased array used in US. The convex array probe is used for example, abdominal examinations since it has a wide imaging area and focusses deeply. For cosmetic dermatology, the linear array probe is recommended because of its superficial focus. Frequency is another characteristic probe. The higher frequency (HF) probes provide more detailed images. However, their penetration depth is limited. So, HF probes ranging from 10-22 MHz are optimally suited for facial examinations. Recently, literature has shown that US can be deployed for vascular mapping, safe placement of fillers and directed low-dose hyaluronidase reversal of vascular adverse events. 8
IS US EASY TO INCORPORATE INTO OUR AESTHETIC PRACTICE?
Yes, US is a noninvasive method that is completed in a few minutes. The use of US requires training and knowledge of anatomy because it is not easy to identify and find the anatomical structures at the beginning. However, several worldwide US academies as Thinkin Academy, Cutaneous, and Sonosthetics teach practitioners how to utilize US for different aesthetic procedures.
ULTRASOUND IN COSMETIC DERMATOLOGY: WHY?
Currently, US is considered the first-imaging technique for dealing with fillers and managing their potential complications. In general, physicians tend to use it for prevention. So, prior to injecting a certain area, they inspect with duplex to detect any arteries are in the way or the presence of anatomical variations are present (Figure 1). In the case of HA filler-related complications, hyaluronidase can be placed with ultrasound-guided injections exactly into the filler deposit. 9,10 In a study by Schelke et al.,9 30-50 units of hyaluronidase were injected into the HA deposits responsible for the occlusion, resulting in immediate restoration of blood circulation, in comparison with high hyaluronidase dose (>500 UI) with high dose protocol not guided by US.9 The incidence of vascular adverse effects after filler injections seems to be 1/6600 (0.015%). US can assist in the identification and evaluation of all the arteries at risk, thus avoiding the occurrence of vascular complications. 11 Although this risk does not seem very high, many injectors even recognized as excellent practitioners, may encounter this event during their career. 12
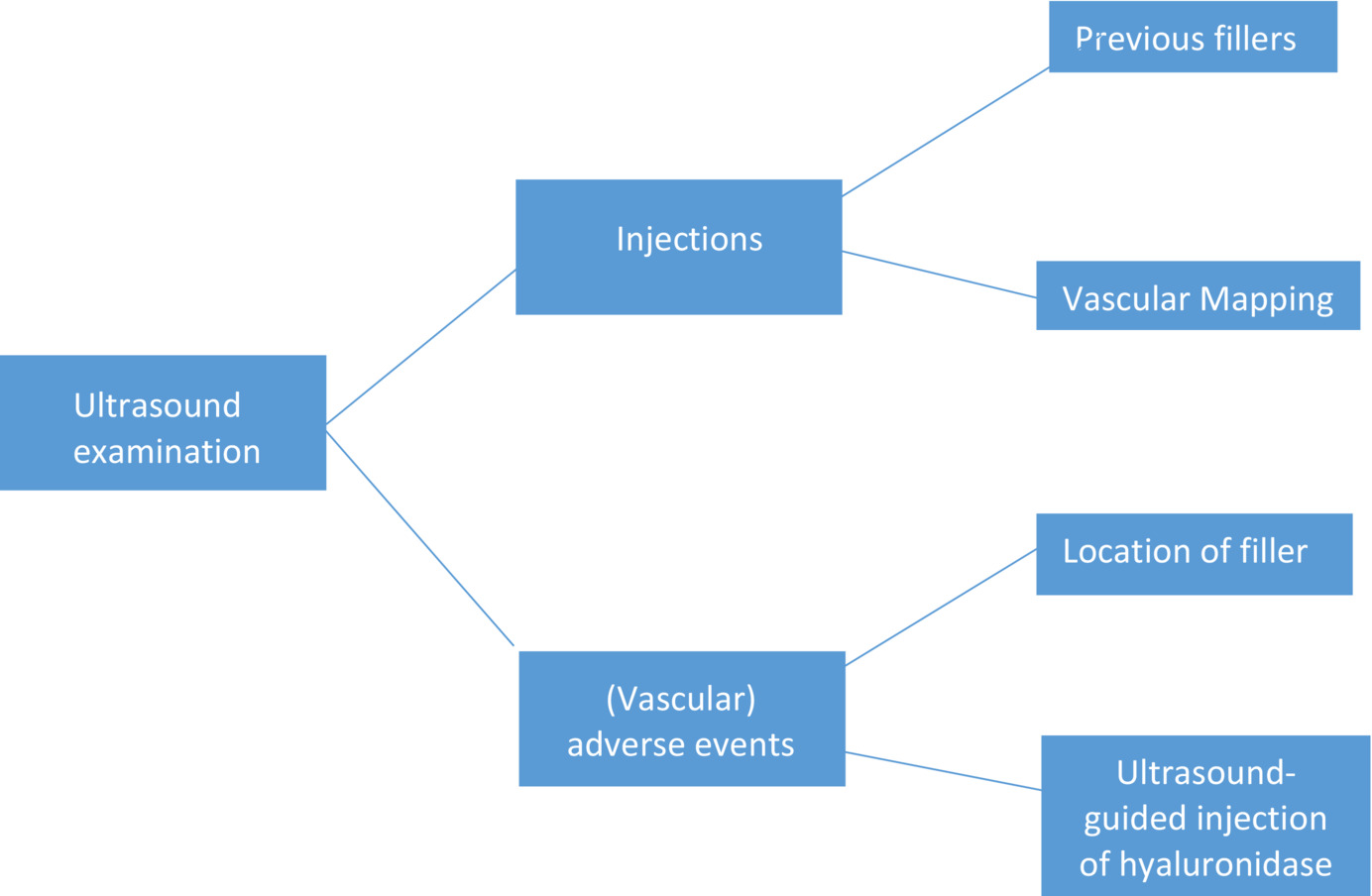
Figure 1. Flow chart describing the potential uses of US in cosmetic dermatology
The use of US is being promoted as a noninvasive imaging modality that provides a good definition for studying the skin and deeper layers in real time, including blood flow, taking us from a static anatomy to a dynamic one. There are many anatomical variations as there are humans.13 For instance, to underscore the variability of lip vasculature, the study by Cotofona et al. 14 shows that the most frequent location of both the Superior and Inferior Labial Artery is the submucosal plane (58.5%) followed by intramuscular (36.2%) and subcutaneous (5.3%) planes. 14
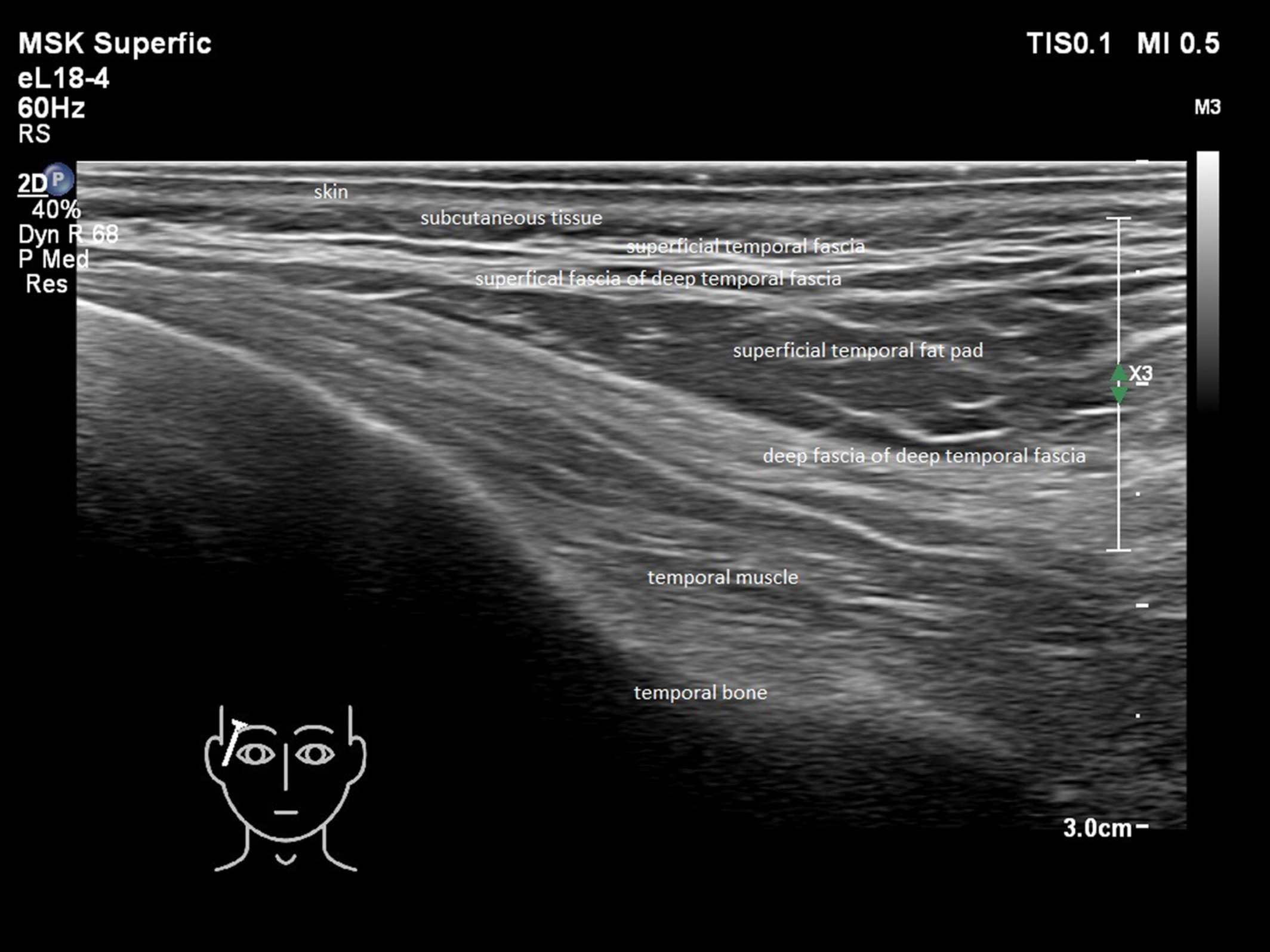
Figure 2. See attachment of picture. The temple is a potential high risk area for injections. In this picture, layers of the temple are visualized by US 18MHz.
Dermal fillers are used widely; some have a permanent effect, whereas others are temporary. Moreover, US has additional advantages such as recognizing remains of previously injected fillers (presence and type). 15-18 Another important application is checking filler treatment execution immediately after injection. Physicians will be able to detect exactly the location of the filler placed.19-22
Based on the US findings in many studies, doctors can be more precise in their guided facial injectable treatments to provide safety for their patients. Based on Cotofona's findings, it seems that the superficial plane of the lower forehead should be avoided due to the unpredictable and inconsistent presence of the central and paracentral arteries. 23 Another practical fact is that a deep supraperiosteal approach should be favored when augmenting the deep midfacial fat compartments. 24 Lastly, it has been shown that in contrast to current concepts, the angular artery is not located strictly subdermal to the nasolabial sulcus but at a variable depth and in 100% of the investigated cases lateral to the nasolabial sulcus. As people age, the depth and lateral distance between arteries and sulci have been shown to reduce. All these variations can easily be seen with US before injection. 25
In addition, US can guide other minimal invasive procedures. To illustrate, US facilitates defining the muscular planes guiding the application of botulinum toxin in patients with bruxism. 26 US may contribute to a more personalized procedure, better cosmetic results, and minimal complications. 27
Last of all, for research purposes, US examination provides valuable information on the behavior, longevity, and interaction of the filler within the tissues.
In conclusion, this new approach for US-guided treatments is a very practical and an effective method in cosmetic dermatology. Keeping the patients out of the harm's way is a doctor's main responsibility, primum non nocere. As physicians, we feel that in the near future, US will be an essential diagnostic tool in any dermatology or cosmetic doctor's office to legally protect the professionals and also to keep the patients safe.
Some testimonials from IMCAS 2022
Dr. Leonie Schelke: “I thought I knew anatomy. I did cadaver courses, I had my books, did injections. But US really made me understand anatomy, visualized the different layers of the skin, I could see the tissue moving, I could relate to different tissue layers, to the mobility, how the filler was looking inside. It's much more than I thought that it would do for safety”.
Dr. Peter Velthuis: “With US imaging we have made the first steps in researching our injectable techniques, but there is so much more to examine. In the next five years, US will fundamentally change the way we conduct our treatments, making them safer but also more effective”.
Dr. Steven Weiner: “I think that US is the ultimate way to examine your patients, even if you're a great anatomist. I use US for safety, for treating complications, for objective measurements for treatments that I do. So US should be included in everyone's practice in the future and will likely become the golden standard for facial injections”.
References
1. Levy J, Barrett DL, Harris N, Jeong JJ, Yang X, Chen SC. High-frequency ultrasound in clinical dermatology: a review. Ultrasound J. 2021;13:24.
2. Wortsman X. Practical applications of ultrasound in dermatology. Clin Dermatol. 2021;39(4):605-623.
3. Wortsman X. Identification and complications of cosmetic fillers: sonography first. J Ultrasound Med. 2015;34(7):1163-1172.
4. Cral WG. Ultrasonography and facial aesthetics. Aesthetic Plast Surg. 2022;46(2):999-1000.
5. Lambros V. Use of Doppler Ultrasound to avoid injection complications. Plast Reconstr Surg. 2019;144(4):724e.
6. Miller JP, Carney MJ, Lim S, Lindsey JT. Ultrasound and plastic surgery: clinical applications of the newest technology. Ann Plast Surg. 2018;80(Suppl 6):S356-S361.
7. Schelke LW, Cassuto D, Velthuis P, Wortsman X. Nomenclature proposal for the sonographic description and reporting of soft tissue fillers. J Cosmet Dermatol. 2020;19(2):282-288.
8. Wortsman X. Ultrasound in dermatology: why, how, and when? Semin Ultrasound CT MR. 2013;34(3):177-195.
9. Schelke LW, Velthuis P, Kadouch J, Swift A. Early ultrasound for diagnosis and treatment of vascular adverse events with hyaluronic acid fillers. J Am Acad Dermatol. 2019;S0190-9622(19):32392-32398.
10. Habib SM, Schelke LW, Velthuis PJ. Management of dermal filler (vascular) complications using duplex ultrasound. Dermatol Ther. 2020;33(4):e13461.
11. Tansatit T, Phumyoo T, Jitaree B, et al. Ultrasound evaluation of arterial anastomosis of the forehead. J Cosmet Dermatol. 2018;17(6):1031-1036.
12. Schelke L, Decates T, Kadouch J, Velthuis P. Incidence of vascular obstruction after filler injections. Aesthet Surg J. 2020;40(8):NP457-NP460.
13. Papadopoulos T. Commentary on: anatomy of the superior and inferior labial arteries revised: an ultrasound investigation and implication for lip volumization. Aesthet Surg J. 2020;40(12):1336-1340.
14. Cotofana S, Alfertshofer M, Schenck TL, et al. Anatomy of the superior and inferior labial arteries revised: an ultrasound investigation and implication for lip volumization. Aesthet Surg J. 2020;40(12):1327-1335.
15. Lee KH, Ryu J, Kim O, et al. Clinical implications of ultrasound artifacts in the cervicofacial area following injection of permanent facial fillers. J Med Ultrason 2001. 2015;42(2):223-229.
16. Schelke LW, Van Den Elzen HJ, Erkamp PPM, Neumann HA. Use of ultrasound to provide overall information on facial fillers and surrounding tissue. Dermatol Surg. 2010;36(Suppl 3):1843-1851.
17. Grippaudo FR, Mattei M. High-frequency sonography of temporary and permanent dermal fillers. Skin Res Technol. 2010;16(3):265-269.
18. Wortsman X, Quezada N. Ultrasound morphology of polycaprolactone filler. J Ultrasound Med. 2017;36(12):2611-2615.
19. Velthuis PJ, Jansen O, Schelke LW, et al. A guide to doppler ultrasound analysis of the face in cosmetic medicine. part 2: vascular mapping. Aesthet Surg J. 2021;41(11):NP1633-NP1644.
20. Velthuis PJ, Jansen O, Schelke LW, et al. A guide to doppler ultrasound analysis of the face in cosmetic medicine. part 1: standard positions. Aesthet Surg J. 2021;41(11):NP1621-NP1632.
21. Rocha PS, Guerra TA, Teixeira DA. Description of a safe doppler ultrasound-guided technique for hyaluronic acid filler in the face—A method to avoid adverse vascular events. J Cosmet Dermatol. 2022;21:2783-2787. doi:10.1111/jocd.14492
22. Lee W, Moon HJ, Kim JS, Yang EJ. Safe glabellar wrinkle correction with soft tissue filler using doppler ultrasound. Aesthet Surg J. 2021;41(9):1081-1089.
23. Cotofana S, Velthuis PJ, Alfertshofer M, et al. The change of plane of the supratrochlear and supraorbital arteries in the forehead-an ultrasound-based investigation. Aesthet Surg J. 2021;41(11):NP1589-NP1598.
24. Schelke L, Velthuis PJ, Lowry N, et al. The mobility of the superficial and deep midfacial fat compartments: an ultrasound-based investigation. J Cosmet Dermatol. 2021;20(12):3849-3856.
25. Gelezhe P, Gombolevskiy V, Morozov S, et al. Three-dimensional description of the angular artery in the nasolabial fold. Aesthet Surg J. 2021;41(6):697-704.
26. Wu WT, Chang KV, Chang HC, et al. Ultrasound imaging of the facial muscles and relevance with botulinum toxin injections: a pictorial essay and narrative review. Toxins. 2022;14(2):101.
27. Quezada-Gaon N, Wortsman X, Peñaloza O, Carrasco JE. Comparison of clinical marking and ultrasound-guided injection of Botulinum type A toxin into the masseter muscles for treating bruxism and its cosmetic effects. J Cosmet Dermatol. 2016;15(3):238-244.
被标记: 激光, 光声电仪 & 非手术塑体
Share this article on


