Removal of Subcutaneous PMMA Nodules Using a 980 nm and 1470 nm Diode Laser (Endolaser)
Keyla Klava, Honório Sampaio Menezes, Gustavo Camargo Silverio, Renata Máira de Godoy Arnony, Fabian Fedrizzi, Alexandre de Jesus Gonçalves Seco, Gabriella Andressa Marchesin Castro
Introduction
Diode lasers (DLs) have been on the market since 1962 and are still considered the most energy-efficient and economical lasers1. Many studies using this equipment have been carried out, demonstrating the ability of DLs to eliminate tumors, polyps, and telangiectasias – with satisfactory effects without causing pain, bleeding, or scars – using a wavelength of 980 nm2. With the same wavelength (980 nm) and tumescent local anesthesia of the fat cells, it was possible to perform a diode laser-assisted lipolysis3.
Concurrently with these studies, we researched methods for the degradation of PMMA using various temperatures. It was found that, for degrading this particle, a temperature of approximately 151 °C was needed.
It is known that layers of collagen and elastin form around PMMA particles. The accumulation of product leads to volume augmentation of these tissues, which are called nodules4.
Based on the aforementioned studies, this work sought to use laser lipolysis techniques with tumescent local anesthesia of the nodules. DLs of 980 nm and 1470 nm were used in continuous mode, so that the tissue formed around the PMMA particle could be degraded then aspirated with a negative pressure syringe-needle.
Case presentation
A patient who had undergone gluteal bioplasty with PMMA administered intramuscularly was selected. A subcutaneous PMMA nodule was confirmed by imaging (ultrasound) in the left lateral gluteal region (figure 1). The patient was placed in the prone position, and tumescent local anesthesia technique was used to administer 2% lidocaine with vasoconstrictor around and inside the nodule (figure 2).
A 16G 1½ needle housing a 600 nm optical fiber (of the diode laser) was inserted into the nodule and lateral to it (figure 3 and 4). Wavelengths of 980 nm at 12 W and 1470 nm at 7 W were used in continuous mode, always making sure that the fiber was inside the nodule to avoid burns. Once the nodule had completely softened, the fiber was removed from inside the needle and a 20-ml syringe was connected to it (figure 5). The material was aspirated using negative pressure and, subsequently, subjected to histopathological examination, confirming it was PMMA.
The study was approved by the Metropolitan University of Santos (Unimes) Research Ethics Committee under protocol number 84759924.9.0000.5509.
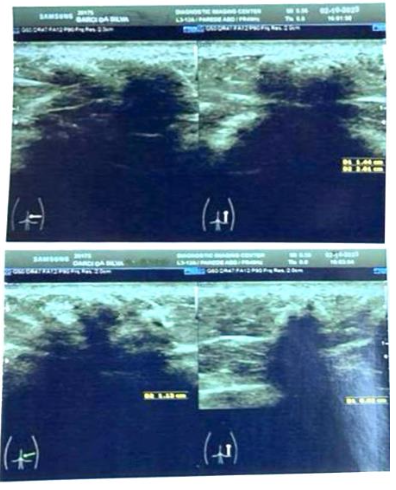
Figure 1: Dermatological ultrasound imaging of PMMA nodules in the subcutaneous tissue.

Figure 2: Intranodular local anesthetic infiltration.
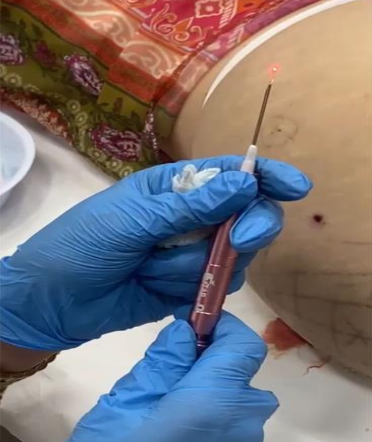
Figure 3: The 600 nm optical fiber of the diode laser housed in a 16G 1½ needle and attached to the handpiece.
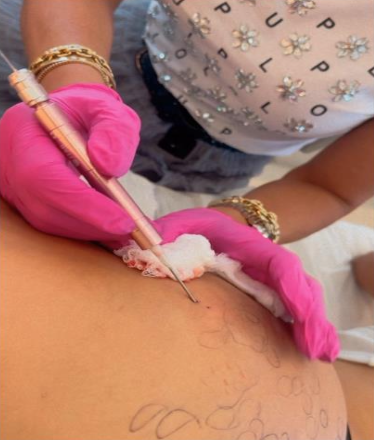
Figure 4: Technical application of the 980 nm and 1470 nm diode laser.
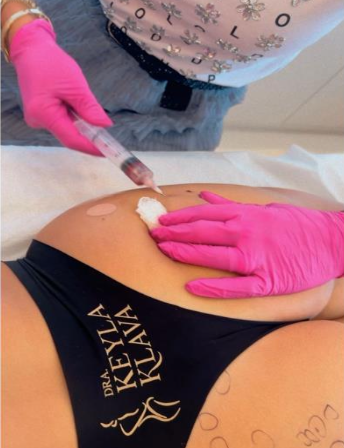
Figure 5: Aspiration of the liquefied nodule using a negative pressure syringe with 20 ml.

Figure 6: Aspirated material
The technique for removing PMMA granulomas from the subcutaneous tissue proved to be efficient. The nodule and surrounding areas had their size reduced, making the region homogeneous. The lump previously present in the area became invisible and impalpable.
The histopathological examination showed collagen fibers, fat cells, and PMMA spheres. The complication was successfully resolved.
Discussion
The safety of PMMA soft tissue fillers in the gluteal region was demonstrated by Chacur et al.5, who found that the risk of complications is below 2% and the incidence of subcutaneous nodules is minimal.
To treat subcutaneous granulomas resulting from the injection of PMMA, we propose the application of a diode laser – firstly tested on the skin in 1962 by Goldman et al. 1. Through time, this type of laser had its technology improved – i.e., low-intensity biostimulation treatments, photobiostimulation, and photodynamic therapy – until it reached the current one in which laser power plays an important role in the outcome6,7.
The several surgical and dermatological applications of diode lasers were extensively discussed by Michalik et al.2.
In 2009, Reynaud et al.3 published a clinical study demonstrating the removal of fat with concurrent subdermal tissue contraction using a 980 nm diode laser. The authors established that enough cumulative energy must be delivered to achieve sufficient lipolysis in the different fat layers3. This observation led us to consider the usefulness of this laser in cases of PMMA accumulation.
The technique used for laser lipolysis is similar to ours, as it consists of the subcutaneous application of the laser under tumescent anesthesia of the treated body region, with or without subsequent aspiration of the liquified fat 8. In this study, however, instead of aspirating fat, we aspirated PMMA particles along with the liquefied vascular tissue and collagen tissue that surround the PMMA microspheres. When the laser comes into direct contact with the tissue surrounding the PMMA, it causes irreversible damage to the adipocytes and thermal damage to the collagen fibers surrounding the PMMA4, breaking down the fibrotic capsules and allowing the aspiration of the liquefied tissue together with the PMMA spheres.
In the present study, a dual 980 nm and 1470 nm diode laser was used, similar to the one previously applied by Wollina and Goldman9 to treat vascular lesions. Since PMMA causes angiogenesis, the effect on the new vessels formed during the accumulation of the filler was expected.
All necessary precautions were taken to protect the adjacent tissue from unintended damage, since the high temperatures of the laser could injury those which are not targeted by the procedure. The use of a needle guide was essential to provide this protection10.
For future studies, we plan to use ultrasound imaging as a potential aid in the correct positioning of the needle and laser fiber, as suggested by Scholten et al.11 and demonstrated by Menezes and Menezes12, who used PMMA for tissue filling in the gluteal region.
This study demonstrated the potential benefits of endolaser application in the treatment of PMMA accumulation with nodule formation in subcutaneous tissue. Therefore, it could be proposed as an alternative to mutilating surgery, which is still performed in many cases.
Conclusion
With the application of 980 nm and 1470 nm diode laser (endolaser), it was possible, effective, and safe to treat subcutaneous PMMA nodules. Without affecting the shape of the tissue and body contour, it is, thus, another therapeutic alternative for treating this complication.
References
1. Goldman L, Blaney DJ, Kindel DJ, et al. Efeito do Raio Laser na Pele. J Invest Dermatol.1963; 40:121–122.
2. Michalik M, Szyma?czyk J, Stajnke M, et al. Medical Applications of Diode Lasers: Pulsed versus Continuous Wave (cw) Regime. Micromachines. 2021; 12:710. doi: 10.3390/mi12060710
3. Reynaud JP, Skibinski M, Wassmer B, et al. Lipolysis using a 980-nm diode laser: a retrospective analysis of 534 procedures. Aesthetic Plast Surg. 2009; 33(1): 28–36. doi: 10.1007/s00266-008-9262-3.
4. Teixeira E, Bortolozzo F, Menezes HS. Biocompatibility and fibrous response of polymethylmethacrylate in skeletal muscles. Int J Dev Res. 2021; 11(10):51034–51039.
5. Chacur R, Menezes HS, Chacur NMB, et al. Gluteal Augmentation with PolymethylMethacrylate: A 10-year Cohort Study. Plast Recons Surg. 2019; 7(5): e2193. doi: 10.1097/GOX.0000000000002193.
6. Mester A. Laser biostimulation. Photomed Laser Surg. 2013; 31: 237–239. doi: 10.1089/pho.2013.9876.
7. Hamblin MR. Photobiomodulation or low-level laser therapy. J Biophotonics. 2016; 9(11-12): 1122–1124. doi: 10.1002/jbio.201670113.
8. Goldman A, Schavelzon DE, Blugerman GS. Laserlipólise: Lipoaspiração com Nd-YAG Laser. Rev Soc Bras Cir Plást. 2002; 17(1): 17–26.
9. Wollina U, Goldman A. The dual 980-nm and 1470-nm diode laser for vascular lesions. Dermatol Ther. 2020; 33(4): e13558. doi: 10.1111/dth.13558.
10. Milanic M, Cenian A, Verdel N, et al. Temperature Depth Profiles Induced in Human Skin In Vivo Using Pulsed 975 nm Irradiation. Lasers Surg Med. 2019; 51(9): 774–784. doi: 10.1002/lsm.23108.
11. Scholten HJ, Pourtaherian A, Mihajlovic N, et al. Improving needle tip identification during ultrasound-guided procedures in anaesthetic practice. Anaesthesia. 2017; 72(7): 889–904. doi: 10.1111/anae.
12. Menezes HS, Menezes OS. Ultrasonography-Guided Cannula Method for PMMA Injection in Aesthetic Gluteal Augmentation. Surg Case Rep. 2023; 5(12): 1–8. doi:10.31487/j.SCR.2022.12.02.
Tagged: Injectables
Share this article on




